Post by Sam Donaldson, Sports and Exercise Physiotherapist
Knee osteoarthritis (OA), is a leading cause of pain and loss of physical function in the knee. Unfortunately, knee OA is an increasing problem in our society, closely linked to our ageing and increasingly overweight population. OA in general is the sixth-ranked most common condition presenting to our GPs.
Knee OA is characterised by joint pain, stiffness and some swelling. It can occur at any age, however it is most common later in life, with some international bodies requiring patients be over 45 in order to be clinically diagnosed.
Often the GP or other health professionals (physios included) may request an X-ray to look at the joint space and congruency of bone surfaces to determine the diagnosis or perhaps the extent of osteoarthritic change.
But what is really going on in there?
Imaging often shows a reduced amount of space between the femur (thigh bone) and tibia (shin bone). There can be other features on the scan as well and some people may say things like, “Oh, that’s bone on bone,” or, “Jeez, there is no space left in there.” This may be correct if we just look at the scan, but it doesn’t necessarily mean you have a problem – or that this problem needs to limit your life plans and goals.
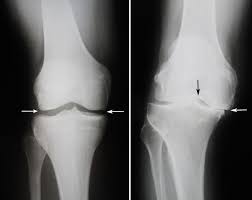
Traditionally, this ‘wear and tear’ of the joint has been considered a very structural and biomechanical problem. This would mean that if you walk or run awkwardly, you are destined to have issues. But more recent research suggests that it’s not that simple.
With increasing weight, there is increasing prevalence of hand OA. Unless people are putting on weight and deciding to walk on their hands, the simple biomechanical explanation for knee OA doesn’t quite fit anymore.
The current explanation involves a more complex combination of normal body processes that involves turnover of our bone and cartilage cells, inflammatory responses, genetics and hormones, as well as our biomechanics.
As we age, the DNA and systems that create new cells when others have exceeded their life-span will create a code that is not as pure as it was in our adolescence and early adulthood. This results in the cartilage and bone gradually become less resilient and durable to new things (like starting to run 5km without prior training = overload).
Being overweight increases a systemic (read: “whole of body”) inflammatory response, which, once it has started in the knee, may continue to occur with this higher systemic state. It may have started with an ACL or Meniscal injury at the age of 15, or simply some boom-bust episodes of exercising over the years, or perhaps your genetic make-up is not as resilient. In any case, attending to this is important.
Finally, there is no ‘perfect movement pattern’, but there are more and less efficient ones and this can be different for everyone. How a person moves determines how forces are distributed around their body – some people naturally move and distribute force well, whereas others unintentionally direct too much force to certain areas of their body. When this excessive force is absorbed by the knee, the result is a structural change of the cartilage within the knee. This feeds into an inflammatory response and causes pain and altered movement or reduced activity, which then results in inconsistent exercise loads and may lead to putting on weight… vicious cycle ensuing…
But it doesn’t need to be a problem that you can’t deal with. As yet, we can’t be sure that the structures can return to normal, but those sources of pain within the knee can absolutely become more resilient and you can get back to living a fulfilling and active lifestyle!